Quick Reference for Schizophrenia
| Feature | Good Outcome | Poor Outcome |
|---|---|---|
| Age | Older | Younger |
| Gender | Female | Male |
| Social class | High | Low |
| Marital history | Married | Never married |
| Family history of schizophrenia | Negative | Positive |
| Perinatal complications | Absent | Present |
| Transcultural factors | Developing nations | Industrialized nations |
| Premorbid functioning | Good | Poor |
| Onset | Acute | Insidious |
| Duration | Short | Chronic |
| Sensorium | Clouded | Clear |
| Symptoms/subtypes | Paranoid subtype | Deficit syndrome |
| Affective symptoms | Present | Absent |
| Neurological functioning | Normal | Soft signs present |
| Neurocognition | Normal | Abnormal |
| Structural brain abnormalities | None | Present |
| When the illness is new, to rule out alternative diagnoses and to stabilize the dose of antipsychotic medication |
| For special medical procedures such as electroconvulsive therapy |
| When aggressive or assaultive behavior presents a danger to the patient or others |
| When the patient becomes suicidal |
| When the patient is unable to properly care for himself or herself (e.g., refuses to eat or take fluids) |
| When medication side effects become disabling or potentially life threatening (e.g., severe pseudoparkinsonism, severe tardive dyskinesia, neuroleptic malignant syndrome) |
| Efficacy |
| Schizophrenia (FDA approved for all) |
| Treatment-resistant schizophrenia (clozapine) |
| Mania (FDA approved for olanzapine) |
| Depression/anxiety/agitation (efficacy established but not FDA approved for these purposes) |
| Side effects |
| Weight gain |
| Sedation |
| Akathisia |
| Orthostatic hypotension |
| Dizziness |
| ↑ Triglycerides |
| EPS, NMS (rare) |
| Agranulocytosis (clozapine) (rare) |
| Seizures (clozapine) |
| Safety in overdose |
| Seizures with clozapine in overdose. Respiratory depression in combination with other CNS depressants. QT interval changes. Lavage and vital sign support |
| Dosage and administration |
| Clozapine: 12.5–25 mg; then increase dosage 25–50 mg per week, as needed and tolerated, to 300–600 mg/day |
| Risperidone: 0.5–1 mg b.i.d. to 3 mg b.i.d. by end of first week, as tolerated |
| Olanzapine: 2.5–5 mg h.s.; increase by 5 mg every week to 20 mg h.s. |
| Quetiapine: 25 mg b.i.d.; increase total daily dose by 50 mg, as needed and tolerated, to 300–600 mg/day |
| Ziprasidone: 20 mg/day or b.i.d.; increase by 20–40 mg per week, to a maximum dosage of 80 mg b.i.d. |
| Aripiprazole: 15 mg/day; increase up to 30 mg/day after 1 week |
| Full benefits in 4 weeks to 6 months |
| Discontinuation |
| Mild cholinergic rebound, faster relapse |
| Taper as slowly as titrated up |
| Drug interactions |
| Fluvoxamine (1A2 inhibitors): ↑ atypical antipsychotic levels |
| EtOH: ↑ sedation and orthostasis |
| Antihypertensives: may ↑ orthostasis |
| Carbamazepine: ↓ serum levels of olanzapine; contraindicated with clozapine |
| CNS depressants: ↑ sedation |
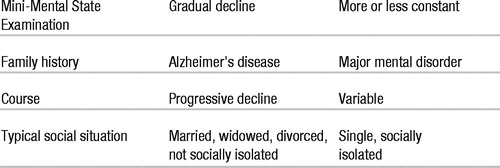 |
Table 4. Typical Antipsychotics: Metabolism and Enzyme Inhibition
| Drug | Major Metabolism Site(s) | Enzyme(s) Inhibited |
|---|---|---|
| Aripiprazole | 2D6, 3A4 | None known |
| Clozapine | 1A2, 3A4, 2D6, 2C19, UGT1A4, UGT1A3 | 2D6a |
| Olanzapine | 1A2, 2D6, UGT1A4, ?other UGTs, ?FMO3 | None known |
| Quetiapine | 3A4, sulfation | None known |
| Risperidone | 2D6, 3A4 | 2D6b |
| Ziprasidone | Aldehyde oxidase, 3A4, 1A2 | None known |
| Women experience more mood symptoms |
| Men experience more deficit symptoms |
| Women present as more socially appropriate |
| Delusional themes differ between the two sexes |
| Men engage in more substance abuse |
| Women have more comorbid problems (allergies, endocrine disturbances, eating disorders, posttraumatic stress disorders, psychophysiological disorders) |
| Symptoms | Alzheimer’s Disease | Schizophrenia |
|---|---|---|
| Delusions | ||
| Someone stealing | +++ | ++ |
| Thought control | +/− | ++/+++ |
| Hallucinations | ||
| Auditory | +/++ | ++/+++ |
| Visual | ++/+++ | + |
| Cognitive impairment | ||
| Short-term memory loss | +++ | + |
| Word-finding difficulties | ++/+++ | −/+ |
| Disorientation | ++ | −/+ |
| Mini-Mental State Examination | Gradual decline | More or lesss constant |
| Family history | Alzheimer’s disease | Major mental disorder |
| Course | Progressive decline | Variable |
| Typical social situation | Married, widowed, divorced, not socially isolated | Single, socially isolated |
| Extrapyramidal Side Effects/Tardive Dyskinesia | Prolactin Elevation | Weight Gain | Glucose Abnormalities | Lipid Abnormalities | QTc Prolongation | Sedation | Hypotension | Anticholinergic Side Effects | |
|---|---|---|---|---|---|---|---|---|---|
| Thioridazine | + | ++ | + | +? | +? | +++ | ++ | ++ | ++ |
| Perphenazine | ++ | ++ | + | +? | +? | 0 | + | + | 0 |
| Haloperidol | +++ | +++ | 0 | 0 | 0 | 0 | ++ | 0 | 0 |
| Clozapinea | 0b | 0 | +++ | +++ | +++ | 0 | +++ | +++ | +++ |
| Risperidone | + | +++ | ++ | ++ | ++ | + | + | + | 0 |
| Olanzapine | 0b | 0 | +++ | +++ | +++ | 0 | + | + | ++ |
| Quetiapinec | 0b | 0 | ++ | ++ | ++ | 0 | ++ | ++ | 0 |
| Ziprasidone | 0b | + | 0 | 0 | 0 | ++ | 0 | 0 | 0 |
| Aripriprazoled | 0b | 0 | 0 | 0 | 0 | 0 | + | 0 | 0 |



