Efficacy of Treatment for Somatoform Disorders: A Review of Randomized Controlled Trials
Abstract
Objective:
To review the evidence from randomized clinical trials (RCTs) that have focused on the treatment of patients with Diagnostic and Statistical Manual of Mental Disorders, 4th Edition (DSM-IV) somatoform disorders. Although somatoform disorders are among the most common mental disorders presenting in the general medical setting, the strength of evidence for specific treatments has not been well synthesized. Methods: MEDLINE search of articles published in English from 1966 to 2006, using the following search terms: randomized clinical trial, somatoform disorders, somatization disorder, undifferentiated somatoform disorder, hypochrondriasis, conversion disorder, pain disorder, and body dysmorphic disorder. Results: A total of 34 RCTs involving 3922 patients were included. Two thirds of the studies involved somatization disorder (n = 4 studies) and lower threshold variants, such as abridged somatization disorder (n = 9) and medically unexplained symptoms (n = 10). Cognitive behavioral therapy (CBT) was effective in most studies (11 of 13), as were antidepressants in a small number (4 of 5) of studies. RCTs examining a variety of other treatments showed benefit in half (8 of 16) of the studies, the most consistent evidence existing for a consultation letter to the primary care physician. Effective treatments have been established for all somatoform disorders except conversion disorder (1 of 3 studies showing benefit) and pain disorder (no studies reported). Conclusion: CBT is the best established treatment for a variety of somatoform disorders, with some benefit also demonstrated for a consultation letter to the primary care physician. Preliminary but not yet conclusive evidence exists for antidepressants.
(Reprinted with permission from Psychosomatic Medicine 2007; 69:881–888)
INTRODUCTION
Somatoform disorders are among the most prevalent mental disorders seen in the general medical setting, present in 10% to 15% of primary care patients (1–4). The functional impairment associated with somatoform disorders is comparable with that seen in depressive and anxiety disorders (5, 6). Moreover, clinically significant somatization leads to excessive health care use, costing the US health care system an estimated $100 billion annually (7). Also, somatoform disorders are among the most frustrating mental disorders for clinicians to manage and also result in high levels of patient dissatisfaction (5, 8–10). Finally, there is greater skepticism regarding the treatability of somatoform disorders compared with the confidence practitioners have regarding the treatment of depression and anxiety. It is likely that if evidence-based treatments existed and were more uniformly applied, the adverse consequences of somatoform disorders, including disability, costs, and dissatisfaction would be reduced.
There have been several evidence-based reviews of psychological treatments for somatic symptoms and functional somatic syndromes (11–15). However, the overlap between these symptom-based general medical disorders and somatoform disorders remains controversial. Therefore, a critical review of the literature was undertaken to determine which treatments are efficacious for somatoform disorders and to ascertain the strength of evidence for particular treatments. The purpose is both to guide current practice as well as to identify gaps in the evidence to inform future treatment research.
METHODS
A MEDLINE search of articles published in English from 1966 to 2006 was conducted, using the following search terms: randomized clinical trial, somatoform disorders, somatization disorder, undifferentiated somatoform disorder, hypochrondriasis, conversion disorder, pain disorder, and body dysmorphic disorder.
Potential studies were also identified from bibliographies of retrieved articles, as well as several recent reviews of selected treatments (12, 14, 16, 17). Prepost studies (i.e., where outcomes were assessed in a single group of patients before and after an intervention) were excluded. Also excluded were studies that focused on specific symptoms (e.g., back pain, headache) or functional somatic syndromes (e.g., irritable bowel syndrome, fibromyalgia).
Data were abstracted on the following key variables: somatoform disorder category, sample size, type of intervention, number of and duration of sessions, type of control group, duration of follow-up, outcomes evaluated, and treatment effect. The following types of patient-centered outcomes were evaluated: a) symptoms (i.e., the study's main measure of somatic symptom count and/or severity); b) functional status (i.e., the study's main measure of functional impairment or quality of life); and c) psychological (i.e., either a domain specific to the disorder, such as hypochondriacal or body dysmorphic beliefs and behaviors, or a generic measure of depression, anxiety, or psychological distress). For each trial, these three outcomes were assessed as positive (outcome was better in the treatment group than the control group), equivocal (there was a trend favoring the treatment group but the group difference was not statistically significant), negative (the groups did not differ), or not assessed. Secondary variables for which data were abstracted include patient demographics (age, gender, educational level, race), and country as well as type of clinic in which the study was conducted.
A standard meta-analytic approach to aggregate the reported data on efficacy was not possible because of the small number of trials for a given intervention within broad treatment classes; substantial differences in the definition and types of reported outcomes; and considerable variation in the reporting of statistical details, such as exact p values and standard deviations. Moreover, many studies neither stated what the primary outcome was nor prespecified the sample size needed to adequately test for a primary outcome. Therefore, similar to several previous literature syntheses of mental health interventions across multiple conditions (12, 18), a vote-counting approach (19) was used to classify each trial as positive or negative. Any trial that reported statistically significant improvement in at least one of the three patient-centered outcomes was operationally defined as a positive trial.
RESULTS
Somatoform disorders studied in the randomized clinical trials
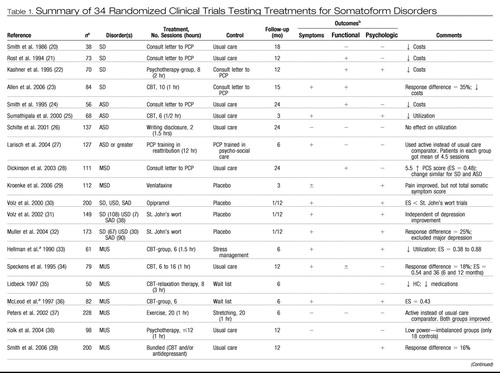
A total of 34 randomized clinical trials (RCTs) involving 3922 patients were included (Table 1). Two thirds of the studies involved somatization disorder (SD) (n = 4 studies) (20–23) and lower threshold variants, such as abridged versions of SD (n = 9) (24–32) and medically unexplained symptoms (n = 10) (33–42). There were five studies of hypochondriasis (43–47), three of conversion disorder (48–50), and three of body dysmorphic disorder (BDD) (51–53). Three of the trials included patients with undifferentiated somatoform disorder (USD) but did not report the results separately for USD (30–32). Also, most or all of the patients in the nine studies of abridged versions of SD and the ten studies of medically unexplained symptoms would likely meet the criteria for USD. Finally, although there are a large number of RCTs in the literature focused on patients with specific pain conditions or chronic pain in general, there were no studies of Diagnostic and Statistical Manual of Mental Disorders, 4th Edition (DSM-IV) pain disorder per se.
 |
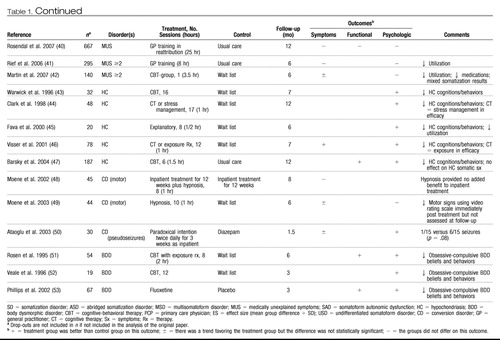 |
Table 1. Summary of 34 Randomized Clinical Trials Testing Treatments for Somatoform Disorders
Treatments studied in the RCTs
Cognitive behavioral therapy (CBT) was the treatment studied in 13 trials, antidepressants in 5, and other treatments in 16 (Table 2). Twelve of the 16 trials involving other treatments were conducted in patients with SD and its lower threshold variants and evaluated a psychiatric consultation letter (n = 4) to the patient's primary care physician (PCP), training PCPs how to better manage somatizing patients (n = 3), non-CBT psychotherapy (n = 2), a multicomponent nurse care management intervention (n = 1), aerobic exercise (n = 1), and writing disclosure (n = 1). There were studies of hypnosis (n = 2) and paradoxical intention (n = 1) in conversion disorder and explanatory therapy (n = 1) in hypochrondriasis.
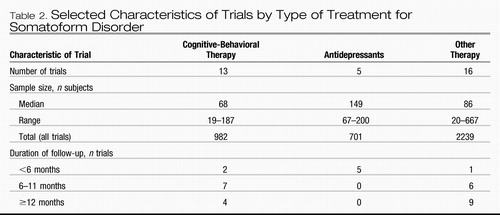 |
Table 2. Selected Characteristics of Trials by Type of Treatment for Somatoform Disorder
The median number of subjects and range per study by type of treatment are shown in Table 2. There were a few studies with very small samples (<40 subjects), and the several largest studies focused on general practitioner training, where patients enrolled were clustered within a modest number of physcians, potentially diminishing the study power. All five antidepressant trials had ≤3 months of follow-up, whereas the duration of follow-up tended to be longer in the studies of nonpharmacological interventions.
Treatment intensity for intervention group and types of control groups
Data could be abstracted for 24 studies (Table 1) on the number of sessions and total contact hours provided for subjects in the intervention arm (it was not relevant and therefore not provided for five antidepressant trials, four trials of a consultation letter to the PCP, and one trial of a bundled CBT/antidepressant trial). The median number of sessions was 8 (range = 1–30), and the median number of total contact hours was 12 (range = 3–25). Subjects in the control arm were assigned to treatment as usual in 12 trials, a wait list in 10, an active comparator in 7, and placebo (all drug trials) in five. The active comparator was a psychiatric consult letter to the PCP in two trials, and stress management, stretching exercises, diazepam, psychiatric inpatient treatment, or specialized PCP psychosocial training in one trial each.
Secondary study characteristics
Slightly over half (n = 18) of the trials reported enrollment rates. In these trials, the median proportion of eligible subjects enrolled was 76% (range = 30%–100%). In the seven CBT trials that reported enrollment rates, the median was 81% (range = 30%–87%). All trials reported the proportion of women, the median being 75% (range = 45%–100%). All trials also reported the average patient age, the median being 43 years (range of average ages = 27.0–50.6 years). Ten trials (all from the United States) reported on race/ethnicity, with the median proportion of minority subjects enrolled being 19% (range = 10%–37%). In the 16 trials that reported educational status, the variable ways of reporting years of schooling made precise pooled estimates difficult. Nonetheless, the median educational level achieved approximated a high school education.
Of the 34 trials, 13 were conducted in the United States (20–24, 28, 29, 33, 36, 39, 47, 51, 53), 6 in Germany (27, 30–32, 41, 42), 6 in the Netherlands (26, 34, 38, 46, 48, 49), 4 in the United Kingdom (37, 43, 44, 52), and 1 each in Denmark (40), Italy (45), Sri Lanka (25), Sweden (35), and Turkey (50). The treatment was administered by a mental health professional (MHP) in 22 trials, a primary care provider in 9 trials (20, 21, 24, 27–29, 39–41), and other types of providers in 3 trials (26, 35, 37). Of the 22 trials involving an MHP-delivered intervention, 10 enrolled subjects solely or predominantly from primary care (22, 23, 25, 33, 34, 36, 38, 42, 45, 47), and the MHPs were psychiatrists in 16 trials (22, 23, 25, 30–32, 34, 43–45, 47–50, 52, 53), psychologists in 4 trials (38, 42, 46, 51), and behavioral medicine specialists in 2 trials (33, 36). Finally, the vast majority of studies were published in the past decade with 22 published since 2000, nine studies between 1995 and 1999, two studies between 1990 and 1994, and only one study before 1990.
Outcomes in general
Outcomes of individual trials are summarized in Table 1. Of the 20 studies assessing somatic symptom outcomes, 10 (50%) were positive trials whereas 4 were equivocal and 6 were negative. Of the 14 studies assessing functional status, 8 (57%) were positive trials whereas 1 was equivocal and 5 were negative. Of the 32 studies assessing psychological distress, 18 (56%) were positive trials whereas 14 were negative. Of the 10 trials in which somatic symptoms improved, depression and/or psychological distress also improved in 7 trials, did not improve in 2 trials, and was not assessed in 1 trial. Improvement in the primary outcome measure was independent of depression status or change in the six studies where this was assessed (31, 32, 39, 44, 45, 53).
A secondary outcome highly relevant to somatoform disorders is health care use and/or costs, and 10 of the 11 studies assessing this outcome showed reduction in health care use (5 trials) or costs (5 trials).
Outcomes by treatment type
Table 3 shows the proportion of positive trials by major treatment category. A positive study was defined as one in which the treatment group fared better than the control group on at least one of the three patient-centered outcomes. The one treatment for which there seems to be convincing evidence is CBT, which proved beneficial for at least one outcome in 11 of 13 trials. Of the five trials examining antidepressants, four were positive (two trials of St. John's wort and one of opipramol for SD-spectrum disorders and one trial of fluoxetine for BDD), whereas one was equivocal for the primary outcome but positive for at least one secondary patient-centered outcome (venlafaxine for SD-spectrum disorders). It should be noted that all antidepressant trials specified a primary outcome, whereas many nonpharmacological studies did not specify a primary outcome but simply reported multiple outcomes.
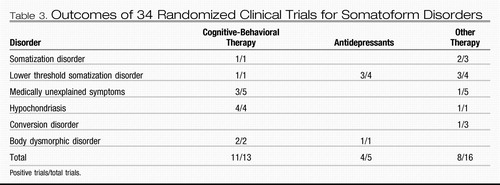 |
Table 3. Outcomes of 34 Randomized Clinical Trials for Somatoform Disorders
Of the other treatments, only two were evaluated in ≥1 or 2 studies. Three of the four trials examining the effectiveness of providing a simple psychiatric consultation letter to PCPs were positive; the benefits were in terms of improved functional status (3 of 4 positive for this outcome) rather than reduced psychological distress (0 of 4 positive). Somatic symptom outcomes were not assessed in any of these four studies, although there were cost savings in all three studies that examined this outcome. Only one of the three trials examining the effectiveness of providing specialized training to PCPs in managing the somatizing patient proved positive.
Outcomes by somatoform disorder category
SD and its lower threshold variants.
CBT was effective in five of seven trials, and antidepressants in three of four trials. A psychiatric consultation letter to the PCP was effective in three of four trials, whereas providing specialized training to the PCP was effective in only one of three trials. A multicomponent nurse-administered intervention, using a type of CBT and antidepressants as indicated, was beneficial in one trial, whereas one of two trials using non-CBT psychotherapy was positive. Finally, one trial found aerobic exercise ineffective (although an active comparator of muscle stretching was used in the control group), and emotional disclosure through writing was ineffective in a single trial.
Hypochondriasis.
CBT proved consistently effective (four of four trials involving a total of 345 patients). One pilot study of explanatory therapy in 20 patients was also positive. All five trials also showed benefits in terms of hypochondriacal cognitions and behaviors.
Body Dysmorphic Disorder.
CBT was effective in two of two trials involving a total of 73 patients, and fluoxetine was effective in a single trial involving 67 patients. All three trials also showed benefits in terms of obsessive-compulsive BDD beliefs and behaviors.
Conversion Disorder.
There were only three small studies of conversion disorder (two using hypnosis and one using paradoxical intention), and the results were inconclusive.
DISCUSSION
This literature synthesis allows one strong and several tentative conclusions regarding the efficacy of treatment for somatoform disorders. First, CBT is consistently effective (11 of 13 trials) across a spectrum of somatoform disorders including SD and its lower threshold variants, hypochondriasis and BDD. Second, a psychiatric consultation letter to the primary care physician about strategies for managing the somatizing patient seems to improve physical functioning (three of four trials) and reduce costs, although surprisingly the effect on somatic symptoms themselves has not been reported. Third, although there is preliminary evidence that antidepressants may be beneficial, the degree to which this is a general effect mediated through reduced depression and anxiety versus a specific effect on somatic symptoms needs to be better ascertained. A variety of other treatments have been evaluated for which the results have been either negative or inconclusive.
All trials except three were published in the past decade. This could be due to a number of factors ranging from substantial changes in classification, a paucity of interest in somatoform disorders, lack of clinical trial funding for these disorders, and the fact that most somatizing patients present in primary care and fewer are referred to mental health specialists than patients with other mental disorders. Although somatoform disorders are just as common as depression and anxiety in primary care, the number and quality of trials to inform our treatment of somatoform disorders are far less.
The literature reviewed has important limitations, which in turn weaken the conclusions we can draw, except for the likely efficacy of CBT. First, the heterogeneity of conditions, disease definitions, treatments, intervention type and intensity, outcomes, and duration of follow-up precluded quantitative pooling of study data. Thus, we had to resort to a crude vote-counting approach of characterizing studies as positive or negative, and a narrative synthesis rather than a formal meta-analysis. Second, most trials measured multiple outcomes and reported neither which outcome was primary nor a prespecified sample size. Therefore, our operational definition of a positive trial as needing to show benefit for only one of the three patient-centered outcomes could overestimate treatment benefits because multiple outcomes were often assessed and analyses were not typically adjusted for multiple hypothesis testing. On the other hand, many studies had small sample sizes meaning the differences that were found had to be of at least a moderate magnitude to be statistically significant. Third, the comparison arm for most studies was a usual care, wait list, or active comparator rather than placebo control. Consequently, blinding of the patient was impossible in many of these studies, and blinding of the outcome assessment was often not specified.
Functional somatic syndromes (e.g., irritable bowel syndrome, fibromyalgia, chronic fatigue syndrome) and individual chronic symptoms (e.g., headache, low back pain) were not the subject of this review but exhibit considerable overlap with somatoform disorders (54) as well as depression and anxiety (55). It is therefore notable that evidence-based reviews have established the efficacy of both CBT and antidepressants for these somatic conditions (11–15, 56). Additionally, it seems the effect of CBT and antidepressants on somatic symptoms is not entirely mediated through reduction of depression and psychological distress (11, 12). On the other hand, depression and anxiety frequently co-occur in patients with functional somatic syndromes as well as somatoform disorders (4, 57), and some studies have suggested that somatic symptoms may improve to a lesser degree than emotional symptoms (58, 59).
Regarding type of treatment, the strongest and most consistent evidence exists for CBT. In contrast, the number of antidepressant trials was small. Of these five trials, four were positive for the prespecified primary outcome, whereas the other was positive for one of the other patient-centered out-comes considered primary for this review. Compared with the nonpharmacological treatment studies, antidepressants had on average larger patient samples, had a prespecified primary outcome, and were placebo-controlled; the latter two factors would tend to increase the likelihood of a negative trial. On the other hand, antidepressant trials tended to have shorter follow-up periods, leaving unanswered questions about the persistence of benefits and the need for chronic therapy. Also, the three antidepressant trials, which showed benefits for SD-spectrum disorders, were all conducted in Germany and used either St. John's wort or opipramolol rather than antidepressants typically prescribed in the US. Much stronger evidence is needed regarding the efficacy of pharmacotherapy, including the magnitude and sustainability of its benefits for somatic symptoms as well as its independent effect not mediated by improvement of comorbid depression and anxiety.
Ironically, a psychiatric consultation letter provided to PCPs was effective in three of four trials, but specialized PCP training was effective in only one of three trials. Although substantial differences between trials make comparisons difficult, several points should be mentioned. First, although the consultation letter trials showed modest improvement in physical functioning, none of the trials reported on somatic symptom outcomes, which is notable in that all four trials were performed in SD or its lower threshold variants. Second, the consultation letter trials were all performed by the same group and had small sample sizes. Nonetheless, the fact that PCP training trials have not shown a convincing effect means further work is needed to determine the optimal balance between PCP care, collaborative care, or referral for CBT for improving outcomes of somatoform disorders in primary care.
In terms of type of somatoform disorder, the most evidence (23 of the 34 trials) (Table 3) exists for the family of related disorders including SD, its abridged or subthreshold variants, and medically unexplained symptoms. Clinical trial evidence for the treatment for other somatoform disorders ranges from modest to limited. The evidence supporting CBT in hypochondriasis is consistent across four trials. Two trials of CBT and one trial of fluoxetine were beneficial in BDD. A meta-analysis of treatments for BDD (60) included, in addition to the RCTs reported here, three case series and one crossover trial of antidepressants (three with SSRI, one with clomipramine) involving 89 patients, and eight case series of psychological treatments (four with behavioral therapy, three with CBT, and one with cognitive therapy) involving 85 patients. Including all studies where the effect size could be derived from the published date, the mean effect sizes were 0.92 for antidepressants (five studies), 1.43 for behavioral therapy (four studies), and 1.78 for CBT (five studies). Effect sizes of 0.8 or greater are considered large therapeutic effects (61). Finally, the three small trials in conversion disorder were inconclusive, yet they are the only trials that qualified for inclusion in a recent Cochrane Collaboration review (62). Although we found no trials focusing on DSM-IV Pain Disorder or Undifferentiated Pain Disorder per se, previous evidence-based reviews of antidepressants, CBT, and other psychological treatments for functional symptoms had patient samples where pain was often a cardinal symptom (11–15, 56). Also, many of the trials in our review that focused on patients with lower-threshold SD and/or medically unexplained symptoms likely included many patients with pain symptoms or undifferentiated SD.
Despite the evidence for some potentially effective treatments, many clinicians find somatoform disorders and medically unexplained symptoms among the most difficult conditions to treat, both in terms of outcomes as well as clinician-patient interactions (10, 63). The reasons for this may be multifactorial including lack of clinician knowledge about evidence-based treatments, lack of access to or inadequate reimbursement for CBT and other psychotherapeutic interventions, concomitant personality disorders, and limited time in busy outpatient encounters with other competing demands. Also, there may be selection bias in published trials. For example, despite the consistent evidence supporting CBT, many such patients seen in clinical practice may refuse referral to mental health providers. Those with somatoform disorders who are convinced their problems are “physical” may be less likely to enroll in studies of “psychological” treatments.
In summary, there is strong evidence supporting the efficacy of CBT across several types of somatoform disorders, and moderate evidence supporting a psychiatric consultation letter in SD and its lower threshold variants. Antidepressants also seem promising, particularly for functional somatic syndromes, but require further study in somatoform disorders per se. The most prevalent type of somatoform disorder is the family of conditions that includes SD, its lower threshold variants including medically unexplained symptoms, USD, and pain disorder. The overlap along a continuum of these disorders with one another and with functional somatic syndromes has important implications for revised classification in DSM-V as well as common treatments (54, 64). Also, psychotherapeutic interventions other than CBT (e.g., interpersonal therapy, problem-solving therapy, brief psychodynamic therapy) as well as treatments outside of what are traditionally considered “psychological” (e.g., optimizing analgesics, the use of pain self-management programs) merit further study for somatoform disorders. Finally, most trials have studied single treatments, whereas it is likely that combining treatments may be necessary in patients with chronic somatic conditions. Because somatoform disorders are as prevalent as depression and anxiety in primary care and account for considerable disability and costs, enhancing treatment outcomes for this often-neglected category of mental disorders should be a priority.
1 Spitzer RL, Williams JB, Kroenke K, Linzer M, deGruy FV III, Hahn SR, Brody D, Johnson JG. Utility of a new procedure for diagnosing mental disorders in primary care. The PRIME-MD 1000 study. JAMA 1994; 272: 1749– 56.Crossref, Google Scholar
2 Ormel J, Vonkorff M, Ustun TB, Pini S, Korten A, Oldehinkel T. Common mental disorders and disability across cultures. Results from the WHO collaborative study on psychological problems in general health care. J. JAMA 1994; 272: 1741– 8.Crossref, Google Scholar
3 Kroenke K, Spitzer RL, Williams JBW. The PHQ-15: validity of a new measure for evaluating the severity of somatic symptoms. Psychosom Med 2002; 64: 258– 66.Crossref, Google Scholar
4 Kroenke K, Rosmalen JG. Symptoms, syndromes, and the value of psychiatric diagnostics in patients who have functional somatic disorders. Med Clin North Am 2006; 90: 603– 26.Crossref, Google Scholar
5 Kroenke K, Spitzer RL, deGruy FV, Hahn SR, Linzer M, Williams JBW, Brody D, Davies M. Multisomatoform disorder: an alternative to undifferentiated somatoform disorder for the somatizing patient in primary care. Arch Gen Psychiatry 1997; 54: 352– 8.Crossref, Google Scholar
6 de Waal MW, Arnold IA, Eekhof JA, van Hemert AM. Somatoform disorders in general practice: prevalence, functional impairment and comorbidity with anxiety and depressive disorders. Br J Psychiatry 2004; 184: 470– 6.Crossref, Google Scholar
7 Barsky AJ, Orav EJ, Bates DW. Somatization increases medical utilization and costs independent of psychiatric and medical comorbidity. Arch Gen Psychiatry 2005; 62: 903– 10.Crossref, Google Scholar
8 Hahn SR, Thompson KS, Wills TA, Stern V, Budner NS. The difficult doctor-patient relationship: somatization, personality and psychopathology. J Clin Epidemiol 1994; 47: 647– 57.Crossref, Google Scholar
9 Hahn SR, Kroenke K, Spitzer RL, Brody D, Williams JB, Linzer M, deGruy FV III. The difficult patient: prevalence, psychopathology, and functional impairment. J Gen Intern Med 1996; 11: 1– 8.Crossref, Google Scholar
10 Jackson JL, Kroenke K. Difficult patient encounters in the ambulatory clinic: clinical predictors and outcomes. Arch Intern Med 1999; 159: 1069– 75.Crossref, Google Scholar
11 O'Malley PG, Jackson JL, Santoro J, Tomkins G, Balden E, Kroenke K. Antidepressant therapy for unexplained symptoms and symptom syndromes. J Fam Pract 1999; 48: 980– 90.Google Scholar
12 Kroenke K, Swindle R. Cognitive-behavioral therapy for somatization and symptom syndromes: a critical review of controlled clinical trials. Psychother Psychosom 2000; 69: 205– 15.Crossref, Google Scholar
13 Jackson JL, O'Malley PG, Kroenke K. Antidepressants and cognitive-behavioral therapy for symptom syndromes. CNS Spectr 2006; 11: 212– 22.Crossref, Google Scholar
14 Allen LA, Escobar JI, Lehrer PM, Gara MA, Woolfolk RL. Psychosocial treatments for multiple unexplained physical symptoms: a review of the literature. Psychosom Med 2002; 64: 939– 50.Google Scholar
15 Raine R, Haines A, Sensky T, Hutchings A, Larkin K, Black N. Systematic review of mental health interventions for patients with common somatic symptoms: can research evidence from secondary care be extrapolated to primary care? BMJ 2002; 325: 1082.Google Scholar
16 Mayou R, Bass C, Sharpe M, editors. Treatment of Functional Somatic Symptoms. Oxford: Oxford University Press; 1995.Google Scholar
17 Looper KJ, Kirmayer LJ. Behavioral medicine approaches to somatoform disorders. J Consult Clin Psychol 2002; 70: 810– 27.Crossref, Google Scholar
18 Kroenke K, Taylor-Vaisey A, Dietrich AJ, Oxman TE. Interventions to improve provider diagnosis and treatment of mental disorders in primary care: a critical review of the literature. P. Psychosomatics 2000; 41: 39– 52.Crossref, Google Scholar
19 Light RJ, Pillemer DB. Summing Up: The Science of Reviewing Research. Cambridge, MA: Harvard University Press; 1984.Google Scholar
20 Smith GR, Monson RA, Ray DC. Psychiatric consultation in somatization disorder: a randomized, controlled study. N Engl J Med 1986; 314: 1407– 13.Crossref, Google Scholar
21 Rost K, Kashner TM, Smith GR. Effectiveness of psychiatric intervention with somatization disorder patients: improved outcomes at reduced costs. Gen Hosp Psychiatry 1994; 16: 381– 7.Crossref, Google Scholar
22 Kashner TM, Rost K, Cohen B, Anderson M, Smith GR Jr. Enhancing the health of somatization disorder patients. Effectiveness of short-term group therapy. Psychosomatics 1995; 36: 462– 70.Crossref, Google Scholar
23 Allen LA, Woolfolk RL, Escobar JI, Gara MA, Hamer RM. Cognitive-behavioral therapy for somatization disorder: a randomized controlled trial. Arch Intern Med 2006; 166: 1512– 8.Crossref, Google Scholar
24 Smith GR, Rost K, Kashner TM. A trial of the effect of a standardized psychiatric consultation on health outcomes and costs in somatizing patients. Arch Gen Psychiatry 1995; 52: 238– 43.Crossref, Google Scholar
25 Sumathipala A, Hewege S, Hanwella R, Mann AH. Randomized controlled trial of cognitive behaviour therapy for repeated consultations for medically unexplained complaints: a feasibility study in Sri Lanka. P. Psychol Med 2000; 30: 747– 57.Crossref, Google Scholar
26 Schilte AF, Portegijs PJ, Blankenstein AH, Der Horst HE, Latour MB, van Eijk JT, Knottnerus JA. Randomised controlled trial of disclosure of emotionally important events in somatisation in primary care. BMJ 2001; 323: 86.Crossref, Google Scholar
27 Larisch A, Schweickhardt A, Wirsching M, Fritzsche K. Psychosocial interventions for somatizing patients by the general practitioner: a randomized controlled trial. J Psychosom Res 2004; 57: 507– 14.Crossref, Google Scholar
28 Dickinson WP, Dickinson LM, deGruy FV, Main DS, Candib LM, Rost K. A randomized clinical trial of a care recommendation letter intervention for somatization in primary care. Ann Fam Med 2003; 1: 228– 35.Crossref, Google Scholar
29 Kroenke K, Messina N, III, Benattia I, Graepel J, Musgnung J. Venlafaxine extended release in the short-term treatment of depressed and anxious primary care patients with multisomatoform disorder. J. J Clin Psychiatry 2006; 67: 72– 80.Crossref, Google Scholar
30 Volz HP, Moller HJ, Reimann I, Stoll KD. Opipramol for the treatment of somatoform disorders results from a placebo-controlled trial. Eur Neuropsychopharmacol 2000; 10: 211– 7.Crossref, Google Scholar
31 Volz HP, Murck H, Kasper S, Moller HJ. St John's wort extract (LI 160) in somatoform disorders: results of a placebo-controlled trial. Psychopharmacology (Berl) 2002; 164: 294– 300.Crossref, Google Scholar
32 Muller T, Mannel M, Murck H, Rahlfs VW. Treatment of somatoform disorders with St. John's wort: a randomized, double-blind and placebo-controlled trial. Psychosom Med 2004; 66: 538– 47.Crossref, Google Scholar
33 Hellman CJC, Budd M, Borysenko J, McClelland DC, Benson H. A study of the effectiveness of two group behavioral medicine interventions for patients with psychosomatic complaints. Behav Med 1990; 16: 165– 73.Crossref, Google Scholar
34 Speckens AEM, van Hemert AM, Spinhoven P, Hawton KE, Bolk JH, Rooijmans GM. Cognitive behavioural therapy for medically unexplained physical symptoms: a randomized controlled trial. BMJ 1995; 311: 1328– 32.Crossref, Google Scholar
35 Lidbeck J. Group therapy for somatization disorders in general practice: effectiveness of a short cognitive-behavioural treatment model. Acta Psychiatr Scand 1997; 96: 14– 24.Crossref, Google Scholar
36 McLeod CC, Budd MA, McClelland DC. Treatment of somatization in primary care. Gen Hosp Psychiatry 1997; 19: 251– 8.Crossref, Google Scholar
37 Peters S, Stanley I, Rose M, Kaney S, Salmon P. A randomized controlled trial of group aerobic exercise in primary care patients with persistent, unexplained physical symptoms. Fam Pract 2002; 19: 665– 74.Crossref, Google Scholar
38 Kolk AM, Schagen S, Hanewald GJ. Multiple medically unexplained physical symptoms and health care utilization: outcome of psychological intervention and patient-related predictors of change. J. J Psychosom Res 2004; 57: 379– 89.Google Scholar
39 Smith, RC, Lyles JS, Gardiner JC, Sirbu C, Hodges A, Collins C, Dwamena FC, Lein C, Given CW, Given B, Goddeeris J. Primary care clinicians treat patients with medically unexplained symptoms: a randomized controlled trial. JGIM 2006; 21: 671– 7.Crossref, Google Scholar
40 Rosendal M, Olesen F, Fink P, Toft T, Sokolowski I, Bro F. A randomized controlled trial of brief training in the assessment and treatment of somatization in primary care: effects on patient outcome. G. Gen Hosp Psychiatry 2007; 29: 364– 73.Crossref, Google Scholar
41 Rief W, Martin A, Rauh E, Zech T, Bender A. Evaluation of general practitioners' training: how to manage patients with unexplained physical symptoms. Psychosomatics 2006; 47: 304– 11.Crossref, Google Scholar
42 Martin A, Fichter MM, Rauh, E, Rief W. A one-session treatment for patients suffering from medically unexplained symptoms in primary care: a randomized clinical trial. Psychosomatics 2007; 48: 294– 303.Crossref, Google Scholar
43 Warwick HM, Clark DM, Cobb AM, Salkovskis PM. A controlled trial of cognitive-behavioural treatment of hypochondriasis. Br J Psychiatry 1996; 169: 189– 95.Crossref, Google Scholar
44 Clark DM, Salkovskis PM, Hackmann A, Wells A, Fennell M, Ludgate J, Ahmad S, Richards HC, Gelder M. Two psychological treatments for hypochondriasis. A randomised controlled trial. Br J Psychiatry 1998; 173: 218– 25.Crossref, Google Scholar
45 Fava GA, Grandi S, Rafanelli C, Fabbri S, Cazzaro M. Explanatory therapy in hypochondriasis. J Clin Psychiatry 2000; 61: 317– 22.Crossref, Google Scholar
46 Visser S, Bouman TK. The treatment of hypochondriasis: exposure plus response prevention vs cognitive therapy. Behav Res Ther 2001; 39: 423– 42.Crossref, Google Scholar
47 Barsky AJ, Ahern DK. Cognitive behavior therapy for hypochondriasis: a randomized controlled trial. JAMA 2004; 291: 1464– 70.Crossref, Google Scholar
48 Moene FC, Spinhoven P, Hoogduin KA, van DR. A randomised controlled clinical trial on the additional effect of hypnosis in a comprehensive treatment programme for in-patients with conversion disorder of the motor type. P. Psychother Psychosom 2002; 71: 66– 76.Crossref, Google Scholar
49 Moene FC, Spinhoven P, Hoogduin KA, van DR. A randomized controlled clinical trial of a hypnosis-based treatment for patients with conversion disorder, motor type. Int J Clin Exp Hypn 2003; 51: 29– 50.Crossref, Google Scholar
50 Ataoglu A, Ozcetin A, Icmeli C, Ozbulut O. Paradoxical therapy in conversion reaction. J Korean Med Sci 2003; 18: 581– 4.Crossref, Google Scholar
51 Rosen JC, Reiter J, Orosan P. Cognitive-behavioral body image therapy for body dysmorphic disorder. J Consult Clin Psychol 1995; 63: 263– 9.Crossref, Google Scholar
52 Veale D, Gournay K, Dryden W, Boocock A, Shah F, Willson R, Walburn J. Body dysmorphic disorder: a cognitive behavioural model and pilot randomised controlled trial. Behav Res Ther 1996; 34: 717– 29.Crossref, Google Scholar
53 Phillips KA, Albertini RS, Rasmussen SA. A randomized placebo-controlled trial of fluoxetine in body dysmorphic disorder. Arch Gen Psychiatry 2002; 59: 381– 8.Crossref, Google Scholar
54 Mayou R, Kirmayer LJ, Simon G, Kroenke K, Sharpe M. Somatoform disorders: time for a new approach in DSM-V. Am J Psychiatry 2005; 162: 847– 55.Crossref, Google Scholar
55 Henningsen P, Zimmermann T, Sattel H. Medically unexplained physical symptoms, anxiety, and depression: a meta-analytic review. Psychosom Med 2003; 65: 528– 33.Crossref, Google Scholar
56 Nezu AM, Nezu CM, Lombardo ER. Cognitive-behavior therapy for medically unexplained symptoms: A critical review of the treatment literature. Behav Ther 2001; 32: 537– 83.Crossref, Google Scholar
57 Kroenke K. Patients presenting with somatic complaints: epidemiology, psychiatric comorbidity and management. Int J Methods Psychiatr Res 2003; 12: 34– 43.Crossref, Google Scholar
58 Greco T, Eckert G, Kroenke K. The outcome of physical symptoms with treatment of depression. J Gen Intern Med 2004; 19: 813– 8.Crossref, Google Scholar
59 Lin EH, Katon W, Von Korff M, Tang L, Williams JW Jr, Kroenke K, Hunkeler E, Harpole L, Hegel M, Arean P, Hoffing M, Della PR, Langston C, Unutzer J. Effect of improving depression care on pain and functional outcomes among older adults with arthritis: a randomized controlled trial. J. JAMA 2003; 290: 2428– 9.Crossref, Google Scholar
60 Williams J, Hadjistavropoulos T, Sharpe D. A meta-analysis of psychological and pharmacological treatments for Body Dysmorphic Disorder. Behav Res Ther 2006; 44: 99– 111.Crossref, Google Scholar
61 Kazis LE, Anderson JJ, Meenan RF. Effect sizes for interpreting changes in health status. Med Care 1989; 27: S178– S189.Crossref, Google Scholar
62 Ruddy R, House A. Psychosocial interventions for conversion disorder. Cochrane Database Syst Rev 2005;( 4): CD005331.Google Scholar
63 Hahn SR. Physical symptoms and physician-experienced difficulty in the physician-patient relationship. Ann Intern Med 2001; 134: 897– 904.Crossref, Google Scholar
64 Kroenke K, Sharpe M, Sykes R. Revising the classification of somatoform disorders: key questions and preliminary recommendations. Psychosomatics 2007; 48: 277– 85.Crossref, Google Scholar



